Food Environments
Background
When you sit at the table with your brothers, sit long, for it is a time that is not counted against you as part of your ordained life span.
– Imam Jafar al-Sadiq
Diet-related disease is a problem of epidemic proportions. Changing people’s diets, however, is easier said than done, and involves more than just telling people what they should eat. That’s because where we eat, and with whom we eat, may be as important (if not more so) for our health as knowing what to eat. For example, children who eat with their families at least three times per week are 35 percent less likely to develop eating disorders, 24 percent more likely to eat healthier foods, and 12 percent less likely to be overweight.1
Our food choices are influenced by personal factors, such as our taste preferences, our emotional states, and how hungry we are. They are also shaped by our environment: the people in our social circles, such as our friends and family; our physical surroundings, including the stores in our communities, the foods they sell, and how much they cost; and other, more indirect influences, such as our exposure to advertising and the government policies that shape the food system. These and other environmental influences are part of what has been called the food environment.
Personal Factors

Studies suggest people tend to eat more, and make less healthy food choices, when they are hungry, stressed, or tired.2,3 These are reasons to get a good night’s sleep and follow a regular eating pattern (i.e., not skipping meals).
Photo credit: GuitarHero188Rock. Creative Commons CC BY-NC-ND 3.0.
Our food choices are influenced by personal factors, such as knowledge, taste preferences, emotional states, and hunger.
Studies suggest people with more knowledge of nutrition tend to make healthier choices.2 Knowledge alone, however, is not enough to remedy poor diets. Even when people are consciously trying to make healthy choices, they have only so much willpower to resist tempting, convenient foods—particularly when hungry, stressed, or tired.2,3
Personal priorities also have an important influence on what people eat. Surveys suggest Americans prioritize taste, cost, nutrition, and convenience (in that order) when making food choices.4 Many consumers also base their food choices on their values, prioritizing their beliefs about public health, environmental stewardship, social justice, or animal welfare, for example. As consumers learn more about these issues, they may be more inclined to “vote with their forks” in favor of agricultural practices that align with their priorities.
What people typically think of as “taste” is actually a combination of taste, smell, and texture.5 Children are born with an innate liking for sweet foods, and combinations of sugar and fat are often particularly appealing.5 People can and do come to appreciate other tastes, however, based on their experiences, and they can develop more of a liking for certain flavors if they are repeatedly exposed to them6,7 Even when we were in the womb, our taste preferences were being shaped by what our mothers ate during pregnancy.8
Social Influences

Studies suggest people mimic the eating behaviors of their friends, families, and co-workers.9 In households where parents regularly eat fruits and vegetables, for example, children are more likely to do the same.10–12
Image copyright.
For better or worse, the people we spend time with affect our food choices.
Studies suggest people mimic the eating behaviors of their friends, families, and co-workers.9 In households where parents regularly eat fruits and vegetables, for example, children were more likely to do the same.10–12 On the same principle, in homes where parents more frequently drank soft drinks, children’s soft drink intake was higher.13 In another study, adults were more likely to increase their fruit and vegetable intake if they had more friends or co-workers who ate at least five servings of fruits and vegetables a day.14
When promoting healthier eating habits, both children and adults tend to respond well to positive encouragement.9 Studies suggest that attempts by parents to control what their children eat, e.g., by withholding access to sweets, tend to backfire. Children in these environments were more likely to desire “restricted” foods, and dislike the healthy foods they were pressured to eat.15 By contrast, studies suggest that when parents set clear guidelines but allow children freedom to choose among healthy options, children adopt healthier eating behaviors.16
The take-home message: Lead by example, and offer positive encouragement.
Food Stores

“There used to be a grocery store on every corner. … Now there's a liquor store on every corner. If you don't have a car, you're in trouble.” – Baltimore City resident
Many of the poorest urban areas in America have lost their supermarkets. In the mid-20th century, middle-class families began migrating to newly built suburbs. Supermarkets followed, relocating to take advantage of cheaper land and cater to more affluent consumers.22,26
Photo credit: Spence Lean. Pigtown: All Things Baltimore, 2009. www.sustainablecitiescollective.com. Used with permission.
Many American families struggle with limited access to healthy food, while in many neighborhoods, candy, soda, and other nutrient-poor foods abound on every street corner. Low-income neighborhoods and communities of color, in particular, tend to have more fast food restaurants, more convenience stores, and fewer supermarkets compared to mostly-white or higher-income communities.17 What do these patterns mean for the diets and health of people who live in those communities?
Researchers can measure the availability of healthy food in communities by surveying stores—checking whether they sell fresh produce, for example. Compared to smaller stores, supermarkets tend to offer the widest variety of healthy options, at the lowest prices.9 Despite these advantages, research shows that simply having access to a supermarket does not necessarily improve diets. Other interventions, such as offering cooking demonstrations and promotional discounts on fruits and vegetables, might encourage people to shop and eat healthier.9,17–21
Even if supermarkets are part of the solution, getting them into places where they are lacking—such as low-income urban areas—can be challenging. Supermarkets require a lot of land, and urban land is often scarce and expensive.22 Store owners have expressed security concerns, and may think they won’t get enough business from lower-income shoppers.22
The reasons people eat what they eat are varied and complex. Access to a vehicle or public transportation, or even the presence of sidewalks, might mean the difference between getting takeout or shopping for groceries. The ways communities are working to improve healthy food access are equally diverse, and include:
- Stocking more fruits and vegetables in corner stores and small grocery stores,
- Ensuring public benefits (e.g., food stamps) can be used at farmers’ markets, and
- Improving public bus routes to supermarkets.23
See also Hunger and Food Insecurity.
Restaurants
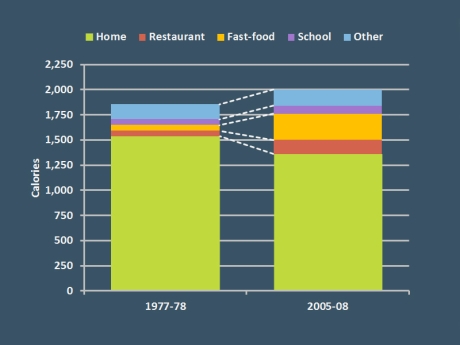
Where do Americans get most of their food?
Between 1977 and 2008, Americans’ share of calories from food prepared away from home increased from 18 to 32 percent.27 Studies suggest meals prepared away from home tend to be less healthy,31 though there are plenty of exceptions.
Data source: National Health and Nutrition Examination Survey (NHANES).
Americans, on average, get roughly one-third of their calories from food prepared at restaurants, cafeterias, and other places away from home.25 The share of calories from fast food restaurants, in particular, has increased dramatically—from 3 to 13 percent—over just three decades.25 An estimated 30 percent of U.S. children now eat at a fast food restaurant daily.26 Why are these trends cause for concern?
Studies suggest people who get more of their meals at restaurants consume more calories, more fat, less fruit, fewer vegetables, and less fiber.27 They may also be at higher risk of weight gain and obesity.28 From 2005 to 2008, meals from fast food restaurants contributed the most saturated fat and the least fiber to American diets, full-service restaurants contributed the most salt, and meals prepared at home were the healthiest on all three counts.29
Restaurants also tend to offer large portion sizes,30 sometimes between two and eight times larger than the standard sizes used in dietary guidelines.31 Sodas, french fries, and hamburgers offered by some fast food chains, for example, are now served in portions between two and six times larger than they were when those items were first introduced.31 Larger portion sizes have been shown to dramatically increase how much consumers eat, often without their realizing it.32
Consumers may not know how much fat and salt are in restaurant items, and tend to vastly underestimate the amount of calories in meals.28 To help address this problem, in 2008 New York became the first city in the U.S. to require menu labeling in restaurants, and in 2010 a federal law was passed requiring chain restaurants to provide menu labels.
School Food

Mixing butternut squash. Nottingham Elementary School, Arlington, Virginia
Efforts to improve school meals face many challenges. Schools may have tight budgets, limited kitchen staff, and (unlike the school pictured here) inadequate kitchen facilities to prepare meals with fresh ingredients. Students, meanwhile, may object—at least initially—to healthier meal offerings when they are accustomed to options like pizza and fries.41
Photo credit: USDA, 2011. Creative Commons CC BY 2.0.
School food environments have been a frequent battleground for competing interests. At stake are the diets and health of American youth, who on average consume more than one-third of their daily calories at school.33
Most public and private schools offer meals through the National School Lunch Program (NSLP), the School Breakfast Program, or both.34 Studies suggest students who participate in federal meal programs consume more fruits, vegetables, and dairy, and are less likely to consume sweetened beverages, desserts, and snacks.33,35 The free and reduced-price meals offered through federal programs also serve as an important safeguard against hunger; nearly 60 percent of children participating in school meal programs come from low-income families.36
When the NSLP was first introduced in 1946, policymakers put restrictions in place to keep private food manufacturers out of schools. Wanting to protect the nutritional quality of school meals, they feared “corporations [would] sell anything to the child as long as he has the money to pay for it.” By the 1970s, however, many school meal programs were short on funding, and private companies could provide meals cheaply and efficiently. Restrictions were lifted, paving the way for fast food chains, soft drink manufacturers, and other private vendors to sell their products—called “competitive foods”—in schools.37
Although competitive foods may generate much-needed funding for schools,36–38 the widespread availability of sugary drinks and high-fat, salty snacks in schools has long been a public health concern.39 The types of competitive foods allowed to be sold in schools, however, are expected to change. In 2010, Congress passed a bill calling for major reform to the school food environment, including setting nutrition standards for competitive foods.40
See also Food Marketing and Labeling.
Resources
The following list of suggested resources is intended as a starting point for further exploration, and is not in any way comprehensive. Some materials may not reflect the views of the Johns Hopkins Center for a Livable Future.
For teachers
- Why We Eat What We Eat (lesson plan). FoodSpan. Johns Hopkins Center for a Livable Future.
- Introduction to the US Food System: Public Health, Environment, and Equity (textbook). Neff RN (editor). Johns Hopkins Center for a Livable Future. 2014.
Reports
- Mapping Baltimore City’s Food Environment: 2015 Report. Johns Hopkins Center for a Livable Future. 2015.
- Researching the Baltimore City Food Environment: Contributions from the Johns Hopkins Bloomberg School of Public Health. Johns Hopkins Center for a Livable Future. 2015.
- Community Food Security in the United States: A Survey of the Scientific Literature. Chen W, Clayton ML, Palmer A. Johns Hopkins Center for a Livable Future. 2015.
- Access to Healthy Food and Why It Matters: A Review of the Research. PolicyLink and The Food Trust. 2013.
- Serving Healthy School Meals. The PEW Charitable Trusts, The Kids' Safe and Healthful Foods Project and the Robert Wood Johnson Foundation. 2013.
- Nutritional Quality of Food Prepared at Home and Away From Home, 1977-2008. USDA Economic Research Service. 2012.
- Healthy Food Access in Minneapolis: Initial Conversations with Residents. Kaiser C. Institute for Agriculture and Trade Policy. 2009.
- Let's Eat Out: Americans Weigh Taste, Convenience, and Nutrition. USDA Economic Research Service. 2006.
Websites
- Healthy Food Access Portal. PolicyLink and The Food Trust.
Academic journal articles
- Dietary Inequalities: What Is the Evidence for the Effect of the Neighbourhood Food Environment? (requires subscription). Black C, Moon D, Baird J. Health and Place. 2014.
- A Framework for Understanding Grocery Purchasing in a Low-Income Urban Environment (free access to research brief). Zachary DA, Palmer AM, et a.. Qualitative Health Research, 2013.
- The Local Food Environment and Diet: A Systematic Review (open access). Caspi CE, Sorensen G, et al. Health & Place. 2012.
- Environmental factors that increase the food intake and consumption volume of unknowing consumers (requires subscription). Wansink B. Annual Review of Nutrition. 2004.
- A Review of Environmental Influences on Food Choices (requires subscription). Larson N, Story M. Annals of Behavioral Medicine. 2009.
Film
- Food Frontiers. Johns Hopkins Center for a Livable Future. 2016.
References
- Hammons AJ, Fiese BH. Is frequency of shared family meals related to the nutritional health of children and adolescents? Pediatrics. 2011;127(6):e1565-e1574.
- Mancino L, Kinsey J. Is Dietary Knowledge Enough? Hunger, Stress, and Other Roadblocks To Healthy Eating. USDA Economic Research Service; 2008.
- Cohen D a, Babey SH. Candy at the cash register - a risk factor for obesity and chronic disease. N Engl J Med. 2012;367(15):1381-1383.
- Glanz K, Basil M, Maibach E, Goldberg J, Snyder D. Why Americans eat what they do: taste, nutrition, cost, convenience, and weight control concerns as influences on food consumption. J Am Diet Assoc. 1998;98(10):1118-1126.
- Drewnowski A. Taste preferences and food intake. Annu Rev Nutr. 1997;17:237-253.
- Sullivan SA, Birch LL. Pass the sugar, pass the salt: Experience dictates preference. Dev Psychol. 1990;26(4):546-551.
- Liem DG, de Graaf C. Sweet and sour preferences in young children and adults: role of repeated exposure. Physiol Behav. 2004;83(3):421-429.
- Mennella JA, Beauchamp GK. Flavor experiences during formula feeding are related to preferences during childhood. Early Hum Dev. 2002;68(2):71-82.
- Larson N, Story M. A review of environmental influences on food choices. Ann Behav Med. 2009;38(1):56-73.
- van der Horst K, Oenema A, Ferreira I, et al. A systematic review of environmental correlates of obesity-related dietary behaviors in youth. Health Educ Res. 2007;22(2):203-226.
- Hanson NI, Neumark-Sztainer D, Eisenberg ME, Story M, Wall M. Associations between parental report of the home food environment and adolescent intakes of fruits, vegetables and dairy foods. Public Health Nutr. 2005;8:77-85.
- Fisher JO, Mitchell DC, Smiciklas-Wright H, Birch LL. Parental influences on young girls’ fruit and vegetable, micronutrient, and fat intakes. J Am Diet Assoc. 2002;102(1):58-64.
- Grimm GC, Harnack L, Story M. Factors associated with soft drink consumption in school-aged children. J Am Diet Assoc. 2004;104(8):1244-1249.
- Sorensen G, Stoddard AM, Dubowitz T, et al. The influence of social context on changes in fruit and vegetable consumption: results of the healthy directions studies. Am J Public Health. 2007;97(7):1216-1227.
- Savage JS, Fisher JO, Birch LL. Parental influence on eating behavior: conception to adolescence. J Law Med Ethics. 2007;35(1):22-34.
- Patrick H, Nicklas T a, Hughes SO, Morales M. The benefits of authoritative feeding style: caregiver feeding styles and children’s food consumption patterns. Appetite. 2005;44(2):243-249.
- Larson NI, Story M, Nelson MC. Neighborhood environments: disparities in access to healthy foods in the U.S. Am J Prev Med. 2009;36(1):74-81.
- Guthman J. Too much food and too little sidewalk? Problematizing the obesogenic environment thesis. Environ Plan A. 2013;45(1):142-158.
- An R, Sturm R. School and residential neighborhood food environment and diet among California youth. Am J Prev Med. 2012;42(2):129-135.
- Boone-Heinonen J, Gordon-Larsen P, Kiefe CI, Shikany JM, Lewis CE, Popkin BM. Fast Food Restaurants and Food Stores. Arch Intern Med. 2014;171(13):1162-1170.
- Cummins S, Flint E, Matthews S a. New neighborhood grocery store increased awareness of food access but did not alter dietary habits or obesity. Health Aff (Millwood). 2014;33(2):283-291.
- Short A, Guthman J, Raskin S. Food deserts, oases, or mirages? Small markets and community food security in the San Francisco Bay area. J Plan Educ Res. 2007;26(3):352-364.
- Treuhaft S, Karpyn A. The Grocery Gap: Who Has Access to Healthy Food and Why It Matters. 2010.
- Gottlieb R, Joshi A. Food Justice. Cambridge, MA: MIT Press; 2010.
- Lin B-H, Guthrie J. Nutritional Quality of Food Prepared at Home and Away From Home, 1977-2008. 2012.
- Bowman S, Gortmaker S, Ebbeling C, Pereira M, Ludwig D. Effects of Fast-Food Consumption on Energy Intake and Diet Quality Among Children in a National Household Survey. Pediatrics. 2004;113(1):112.
- Saelens BE, Glanz K, Sallis JF, Frank LD. Nutrition environment measures study in restaurants (NEMS-R): development and evaluation. Am J Prev Med. 2007;32(4):273-281.
- Story M, Kaphingst KM, Robinson-O’Briend R, Glanz K. Creating Healthy Food and Eating Environments: Policy and Environmental Approaches. Annu Rev Public Heal. 2008;29:253-272.
- Stewart H, Blisard N, Jolliffe D. Let’s Eat Out: Americans Weight Taste, Convenience, and Nutrition. USDA ERS. 2006. http://www.ers.usda.gov/publications/eib-economic-information-bulletin/eib19.aspx
- Story M, Kaphingst KM, Robinson-O´Brien R, Glanz K. Creating healthy food and eating environments: policy and environmental approaches. Annu Rev Public Health. 2008;29:253-272.
- Young LR, Nestle M. Expanding portion sizes in the US marketplace: implications for nutrition counseling. J Am Diet Assoc. 2003;103(2):231-234.
- Wansink B. Environmental Factors that Increase the Food Intake and Consumption Volume of Unknowing Consumers. Annu Rev Nutr. 2004;24:455-479.
- Briefel RR, Wilson A, Gleason PM. Consumption of low-nutrient, energy-dense foods and beverages at school, home, and other locations among school lunch participants and nonparticipants. J Am Diet Assoc. 2009;109(2 Suppl):S79-S90.
- Fox MK, Hamilton W, Lin B-H. Effects of Food Assistance and Nutrition Programs on Nutrition and Health: Volume 3, Literature Review. Washington DC; 2004.
- Mancino L, Todd JE, Guthrie J, Lin B-H. How Food Away From Home Affects Children’s Diet Quality. 2010.
- Story M, Kaphingst KM, French S. The role of schools in obesity prevention. Futur Child. 2006;16(1, Childhood Obesity):pp. 109-142.
- Levine S. School Lunch Politics: The Surprising History of America’s Favorite Welfare Program. Princeton, NJ: Princeton University Press; 2008.
- U.S. Government Accounting Office. School Meal Programs: Competitive Foods Are Widely Available and Generate Substantial Revenues for Schools. Washington, DC; 2005.
- Story M, Nanney MS, Schwartz MB. Schools and Obesity Prevention: Creating School Environments and Policies to Promote Healthy Eating and Physical Activity. Milbank Q. 2009;87(1):71-100.
- USDA Food and Nutrition Service. The School Day Just Got Healthier. 2013. http://www.fns.usda.gov/healthierschoolday.
- Poppendieck J. Free for All: Fixing School Food in America. Berkeley, CA: University of California Press; 2010.
